The gastroduodenal artery is a key player in stomach vascular anatomy, yet it is often omitted from discussions of surgical approaches and diagnostics. Despite its essential role in supplying blood to vital regions, such as the stomach, duodenum, and pancreas, this artery’s significance cannot be underestimated, particularly in cases of bleeding or injury along its surgical route. Understanding the particular region and characteristics of the abdomen is crucial for clinicians and surgeons practicing abdominal surgery.
In surgical practice, damage to the gastroduodenal artery can bring about awesome complications, along with lifestyles-threatening hemorrhages. Surgeons need to be aware of its anatomy to avoid accidental damage, especially during procedures involving the pancreas or surrounding tissues. Diagnostic imaging, which incorporates CT scans and ultrasounds, is also based on clear facts about the artery’s direction to ensure accurate analysis and treatment plans for patients with gastrointestinal troubles.
For radiologists and medical experts, statistics on the gastroduodenal artery’s features are as vital in diagnostics as they are in surgical treatment. Its involvement in positive pathologies, like peptic ulcers or tumors, warrants eager attention in the route of imaging. Knowing how to identify this artery on several scans not only permits treating current situations but also prevents potential complications in future surgical procedures or diagnostic techniques.
Anatomy of the Gastroduodenal Artery: Location and Structure
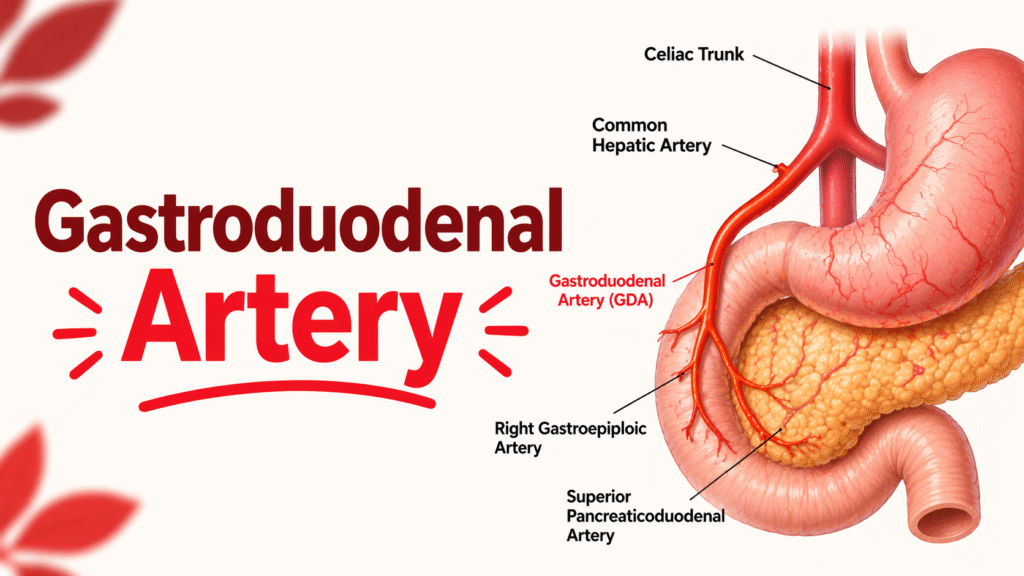
The gastroduodenal artery originates from the common hepatic artery; it is, without a doubt, itself a department of the celiac trunk. It runs downward and to the right, passing through the back of the duodenum to deliver blood to the stomach and higher gut. The GDA gives rise to numerous key branches that feed the gallbladder, stomach and pancreas, alongside the right gastroepiploic artery, which serves the greater curvature of the stomach.
Its vicinity is pivotal in stomach surgical strategies. For instance, the GDA lies close to systems such as the pancreas, duodenum, and bile ducts, making it vulnerable to future damage if strategies that incorporate pancreaticoduodenectomy or duodenal surgery are used. Understanding its course is important for preventing unintended harm that could lead to severe complications, such as hemorrhage.
In addition to its anatomical role, the gastroduodenal artery’s function extends beyond blood delivery. It’s also a critical player in preserving proper gastrointestinal function. Its proximity to vital one-of-a-kind arteries, such as the superior mesenteric artery and the splenic artery, ensures that the digestive organs receive the oxygenated blood they need for optimal, reliable and overall performance.
Clinical Significance of the Gastroduodenal Artery in Surgery
The gastroduodenal artery’s clinical significance becomes more pronounced during stomach surgery, particularly when the pancreas or duodenum is involved. Damage to the GDA can lead to catastrophic bleeding, posing a significant risk to the patient’s safety. Surgeons performing pancreatic surgical strategies want to be acutely aware of the GDA’s region, as unintended damage should bring about hemorrhage that’s hard to control.
A famous case of GDA headaches occurred in the course of a complex pancreaticoduodenectomy, in which an affected person experienced massive bleeding due to a severed GDA. The surgical institution needed to speedily perform a ligation to stop the bleeding, demonstrating how crucial it is to avoid injuring this artery. This event highlights the need for specific knowledge of GDA anatomy to minimize such complications.
In addition to its involvement in predominant surgical procedures, the GDA’s proximity also affects its role in laparoscopic approaches, where careful navigation around key stomach arteries is crucial to avoid inadvertent damage. Surgeons use imaging technologies to pinpoint its location, thereby minimizing patient risk.
Gastroduodenal Artery and Abdominal Bleeding: A Silent Risk
One of the greatest dangers of the gastroduodenal artery is its potential involvement in gastric bleeding. When the GDA is broken, in particular in times of trauma or peptic ulcers, the result can be severe hemorrhaging. This frequently occurs when the GDA is the primary source of blood to the duodenum and the pancreas, each of which can be susceptible to ulcers or damage. A common scenario is the affected character with a bleeding peptic ulcer, in which the GDA is eroded by gastric acid or ulceration.
This can cause life-threatening bleeding, requiring urgent intervention. In such instances, endoscopic strategies or surgical techniques are employed to manipulate the bleeding. Understanding how the GDA assets bleed to these regions allows clinicians to better manage the supply-demand imbalance, which is why it y important to do so more quickly and effectively.
Intraoperative identification of the GDA is important in certain conditions, as failure to address this artery can result in uncontained bleeding and subsequent headaches. Surgeons frequently use intraoperative Doppler ultrasound or, certainly, one of the advanced imaging modalities to detect and repair injuries to the GDA during the procedure.
Imaging the Gastroduodenal Artery: Diagnostic Approaches
Accurate imaging of the gastroduodenal artery is vital for diagnosing conditions involving it and guiding surgical strategies. Several diagnostic imaging strategies, including CT, MRI, and ultrasound, are used to visualise the GDA’s region and integrity.
For instance, CT angiography is normally used to assess the GDA and its branches, specifically in patients with trauma or gastrointestinal bleeding. This non-invasive technique provides high-resolution snapshots, allowing clinicians to detect ruptures, blockages, or aneurysms in the GDA and its branches. By using advanced imaging, clinicians can plan surgeries more effectively, avoiding unnecessary damage to the artery during interventions.
In addition to CT and MRI, endoscopic ultrasound (EUS) has been established as a great tool for visualizing the GDA in patients undergoing exams for peptic ulcers or other gastrointestinal conditions. It allows doctors to have a real-time understanding of the artery’s condition and associated risks.
Risk’s diagnostic strategies are effective substitutes. However, effectiveness hinges on a clinician’s understanding of GDA anatomy and capability variations, which can affect the Gastroduodenal Artery in Peptic Ulcer Disease
The gastroduodenal artery plays a pivotal role in peptic ulcer disease, specifically when ulcers are positioned near the stomach or duodenum. These ulcers can erode into the artery, causing severe bleeding. In fact, the GDA is one of the most common sources of bleeding in sufferers with peptic ulcers, specifically people who present with a history of gastric or duodenal ulcers.
When an affected person presents with a perforated ulcer, surgeons need to be prepared to deal with active bleeding from the GDA, as failure to control the hemorrhage can result in death or loss of life. Understanding the relationship between some of the GDA allows surgeons to identify sources of blemish more quickly, reducing the time required to perform surgical interventions.
In times when endoscopy is used to deal with bleeding ulcers, the gastroduodenal artery’s circumstances need to be cautiously monitored. Techniques like endoscopic banding or injection treatment can be used to control bleeding, but knowledge of where the GDA is located remains important for successful treatment.
Variations in the Gastroduodenal Artery: Clinical Relevance
Like many arteries, the gastroduodenal artery can exhibit variations in its anatomy. These versions are essential to keep in mind throughout every diagnostic and surgical strategy. For example, in a few instances, the GDA may ariseommon hepatic artery, at the same time frm a more common hepatic artery.
The incidence of those variations is quite low; however, information about them is essential, especially during surgical interventions. Surgeons who are unaware of those versions may also inadvertently injure the artery or bypass over an essential anatomical anomaly that would affect surgical outcomes. Preoperative imaging plays a significant role in identifying the various versions, allowing the surgical team to tailor their technique accordingly.
In unusual instances, the GDA can also have additional branches or an extraordinary route that makes it more inclined in the course of surgical techniques. This highlights the need for an in-depth study of the gastroduodenal artery’s anatomy, even though it seems to be a regular element of the belly’s anatomy.
The Gastroduodenal Artery in Endoscopic Procedures and Surgery
Endoscopic strategies, including laparoscopy or endoscopic retrograde cholangiopancreatography (ERCP), require cautious navigation of the abdominal vasculature, including the gastroduodenal artery. Surgeons must ensure they no longer inadvertently harm the GDA during these minimally invasive procedures.
One example is all through laparoscopic cholecystectomy, wherein the general practitioner needs to be cautious not to reduce or cauterize the GDA whilst disposing of the gallbladder. Understanding the GDA’s location is vital to warding off inadvertent damage, which could lead to additional bleeding.
Endoscopic ultrasound (EUS) is likewise a valuable tool within diagnostic endoscopic strategies to visualize the GDA, making sure it is not inadvertently injured. In many instances, determining the GDA before starting the process allows for a more stable, more effective treatment.
Key Surgical and Diagnostic Takeaways for the Gastroduodenal Artery
To summarize, understanding the anatomy and function of the gastroduodenal artery is important for every surgical procedure and correct evaluation. Surgeons and clinicians have to be organized to apprehend the GDA during stomach procedures, as harm to this artery can bring about massive complications, together with bleeding or problems with tissue restoration.
Diagnostic professionals, in particular radiologists and gastroenterologists, need to prioritize identifying the GDA within a few unspecified time in the future of imaging strategies to prevent errors.
By combining a solid understanding of its anatomical route with cutting-edge diagnostic and surgical strategies, clinical professionals can improve patient outcomes and reduce headaches associated with GDA injuries or abnormalities.
Conclusion: Ensuring Safety and Accuracy with the Gastroduodenal Artery
The gastroduodenal artery can be small, but its function in each surgical operation and diagnostic procedure is substantial. From its involvement in peptic ulcer disorder to its significance in stomach surgeries, the GDA’s characteristics can not be disregarded.
Understanding its anatomy, variations, and clinical implications is essential for reinforcing surgical fulfillment and patient care. By adopting a multidisciplinary approach that includes correct imaging, preventive measures ultimately of surgery, and clinical understanding, healthcare vendors can ensure more secure outcomes for sufferers requiring belly techniques.
Frequently Asked Questions
What is the location of the gastroduodenal artery in stomach surgical treatment?
The GDA is important for supplying blood to the stomach, duodenum, and pancreas. Its damage in the direction of stomach surgical procedures, together with pancreatic surgical treatment, can cause excessive bleeding, requiring prompt control.
How does the gastroduodenal artery relate to peptic ulcer illness?
In peptic ulcer disease, the GDA can be eroded by ulcers, leading to bleeding. It is one of the most common symptoms of bleeding in sufferers with ulcers located close to the duodenum or stomach.
Why is the gastroduodenal artery essential in diagnostic imaging?
Accurate imaging of the GDA is important for diagnosing bleeding or anatomical abnormalities. Techniques like CT angiography or endoscopic ultrasound assist clinicians in visualizingin visualizing the artery and planning interventions.
What are the common versions of the gastroduodenal artery’s anatomy?
The GDA can also exhibit anatomical variations, originating from the superior mesenteric artery or having additional branches. These variations are uncommon but crucial to recognize before surgical treatment or imaging.
How can I keep away from the unfavorable gastroduodenal artery at some point of surgical treatment?
Surgeons can avoid GDA injury by thoroughly understanding its anatomical course, using imaging guidance throughout the procedure, and taking extra precautions when performing surgical techniques involving the pancreas or duodenum.